What is Parkinson’s Disease?
Parkinson’s is a progressive nervous system disorder that affects movement, which is thought to affect around 1 in 500 people, most of whom are over the age of 50.
It is primarily characterised by:
- involuntary shaking of particular parts of the body (tremor)
- slow movement
- stiff and inflexible muscles
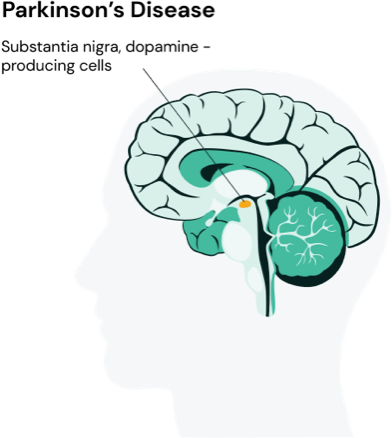
How does Parkinson’s work?
Parkinson’s is caused by atrophy of nerve cells in part of the brain called the substantia nigra. This leads to a reduction in a chemical called dopamine in certain parts of the brain. The reduction in dopamine is responsible for many of the symptoms of Parkinson’s disease, as it plays a vital role in regulating movement. The cause of the cell death in the substantia nigra is poorly understood, but involves the build-up of misfolded proteins into Lewy bodies in the neurons.
How can Parkinson’s be treated?
Clinical case studies are also being prepared for publication which will be posted here soon.
If you would like to discuss TPS® Parkinson’s treatment with one of our expert clinicians, please contact us using the details below.
Get in Touch